Doctor’s Guide: 7 Evidence-Based Ways to Cut Allergy Symptoms This Spring
7 practical protocols to cut symptoms, medication use, and misery
Every spring, it starts the same way.
I step outside on one of those perfect early-April mornings, sun on my face, birds out, everything blooming. And within an hour, my eyes are swollen, my nose starts running, and I’m sneezing so frequently that my friends start to look concerned.
In medical school, I did what most people do: I grabbed whatever antihistamine was in the medicine cabinet. But the side effects were not trivial. My mouth got so dry I was constantly sipping water through lectures. My eyes, already itchy from pollen, became even drier and I had to stop wearing contact lenses. I remember sitting in pharmacology class, ironically learning about the anticholinergic effects of the very drug I was taking, while experiencing them myself.
That frustration is what pushed me into the research. This article is the approach I take: where I start with the most useful first-line measures, then add optional layers based on symptoms and how much effort I want to put in.
1. Daily Nasal Saline Irrigation
Saline is incredibly underrated and the mechanism is simple: it helps clear mucus and wash out allergens from the nasal cavity.
A 2018 Cochrane review found that saline irrigation produced large reductions in allergy symptom severity, though the overall certainty of evidence was rated low to very low due to small, heterogeneous trials (Head et al., 2018).
A 2012 meta-analysis of 10 RCTs found a 28% improvement in nasal symptoms and a 62% reduction in medication use (Hermelingmeier et al., 2012).
The Protocol:
Squeeze bottle (like NeilMed Sinus Rinse) or neti pot, once or twice daily
Use pre-made saline packets
Always use distilled, sterile, or previously boiled water. Never tap water.
Irrigate twice daily or after coming indoors from heavy pollen exposure
When you’re busy: A full rinse takes a few minutes and some setup. On hectic mornings or late nights, I grab a pressurized saline canister and do a quick spray in each nostril. Sometimes I’ll even use it in the shower. Not as thorough as a full rinse, but far better than skipping it.
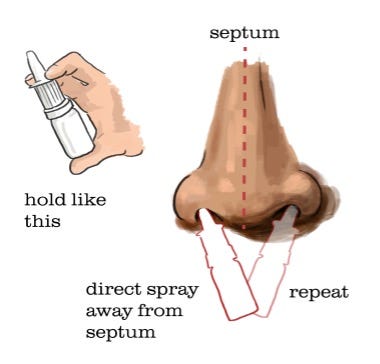
2. Intranasal Steroids
While antihistamines mainly target histamine, intranasal steroids suppress multiple inflammatory pathways in your nasal mucosa, which is why they work better for congestion.
The 2015 AAO-HNS clinical practice guideline made a strong recommendation that intranasal corticosteroids should be first-line therapy for allergic rhinitis affecting quality of life (Seidman et al., 2015).
A 2022 meta-analysis of 8 RCTs (882 participants) confirmed that daily use was significantly more effective than as-needed use for symptom scores, quality of life, sneezing, and congestion (Hoang et al., 2022).
The Protocol:
Start 1-2 weeks before allergy season (these take days to reach full effect)
Use a nasal steroid recommended by your physician (some are available over the counter, but always best to check with your doctor before starting)
Aim the nozzle away from your septum and sniff gently
I use daily through the season, not just on bad days
3. Second-Generation Antihistamines
Antihistamines block histamine receptors to reduce sneezing, itching, and runny nose, but they do not address the broader inflammation that causes congestion.
The same 2015 guideline gave a strong recommendation for second-generation oral antihistamines specifically for sneezing and itching (Seidman et al., 2015).
Second-generation options (e.g., cetirizine) are far less sedating than older options like Benadryl, with fewer anticholinergic side effects.
The Protocol:
If sneezing and itching are prominent, add a second-generation antihistamine daily during allergy season
If congestion is the main problem, intranasal steroids alone may be sufficient
Because long-term cumulative exposure to strong anticholinergic medications has been associated with dementia risk in older adults, I prefer to use the lowest necessary dose and avoid routine use of older, more anticholinergic antihistamines when possible (Coupland et al., 2019).
4. Optimize Your Bedroom Air
Reducing airborne allergen exposure in the room where you sleep 7 to 9 hours can lower your overnight allergen load and improve sleep, even if daytime symptom improvement is harder to improve.
HEPA filters are designed to capture at least 99.97% of 0.3-micron particles, but translating that into consistent symptom relief has been difficult to demonstrate in clinical trials. I view bedroom air control as a practical adjunct, not a core evidence-based treatment.
The Protocol:
I keep a HEPA purifier in my bedroom, running continuously during allergy season
Keep windows closed on high-pollen days
Shower and change clothes when you come inside
Wash bedding in hot water weekly
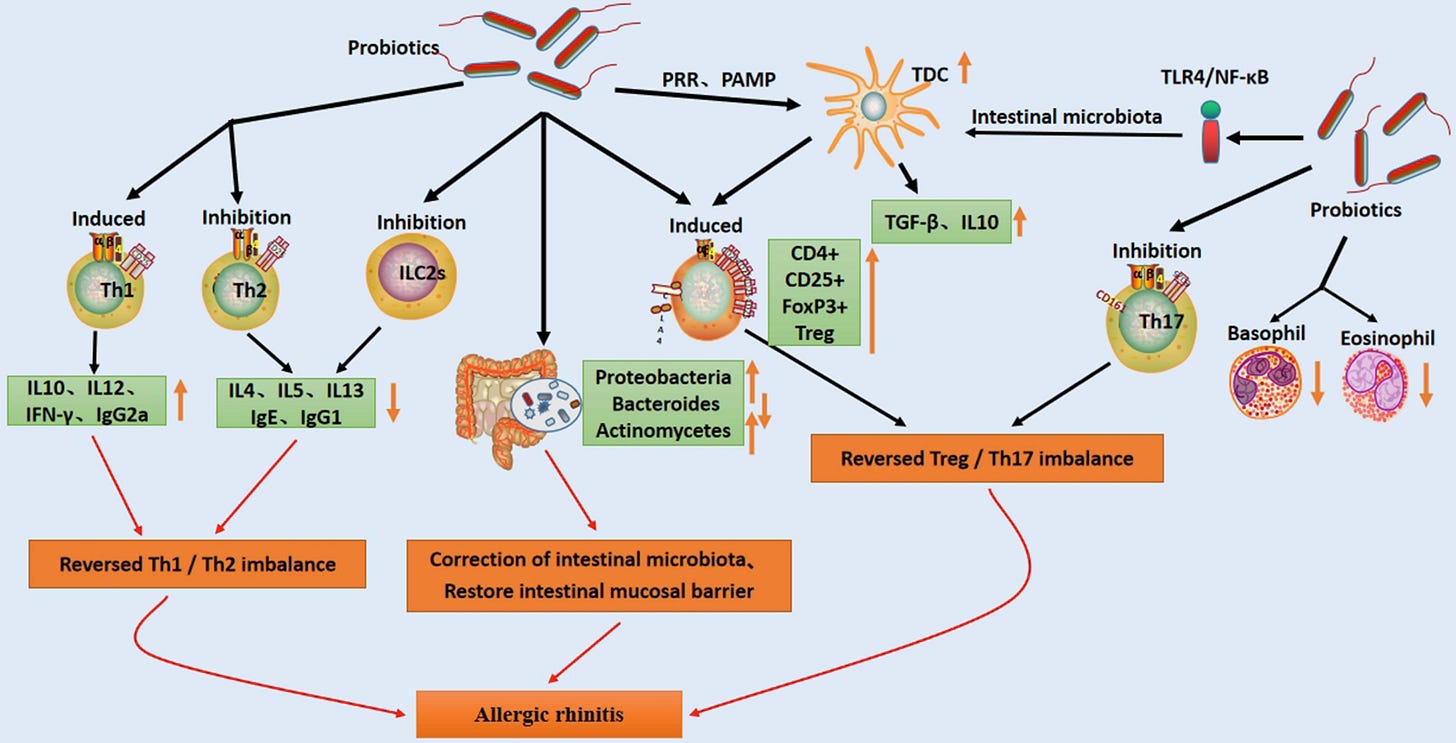
5. Probiotics as an Adjunct
Probiotics may nudge the immune system away from the Th2-skewed (allergic) response through the gut-immune axis, though evidence is still early.
Two 2022 meta-analyses (28 and 30 RCTs respectively) both found improvements in allergy symptoms and quality of life with probiotics, but both reported very high study-to-study variability (Luo et al., 2022; Yan et al., 2022).
No optimal strain or dose has been established.
The Protocol:
If you want to try them, treat probiotics as an optional add-on
Trials have most often used Lactobacillus and Bifidobacterium strains
No optimal strain, dose, or timing has been established
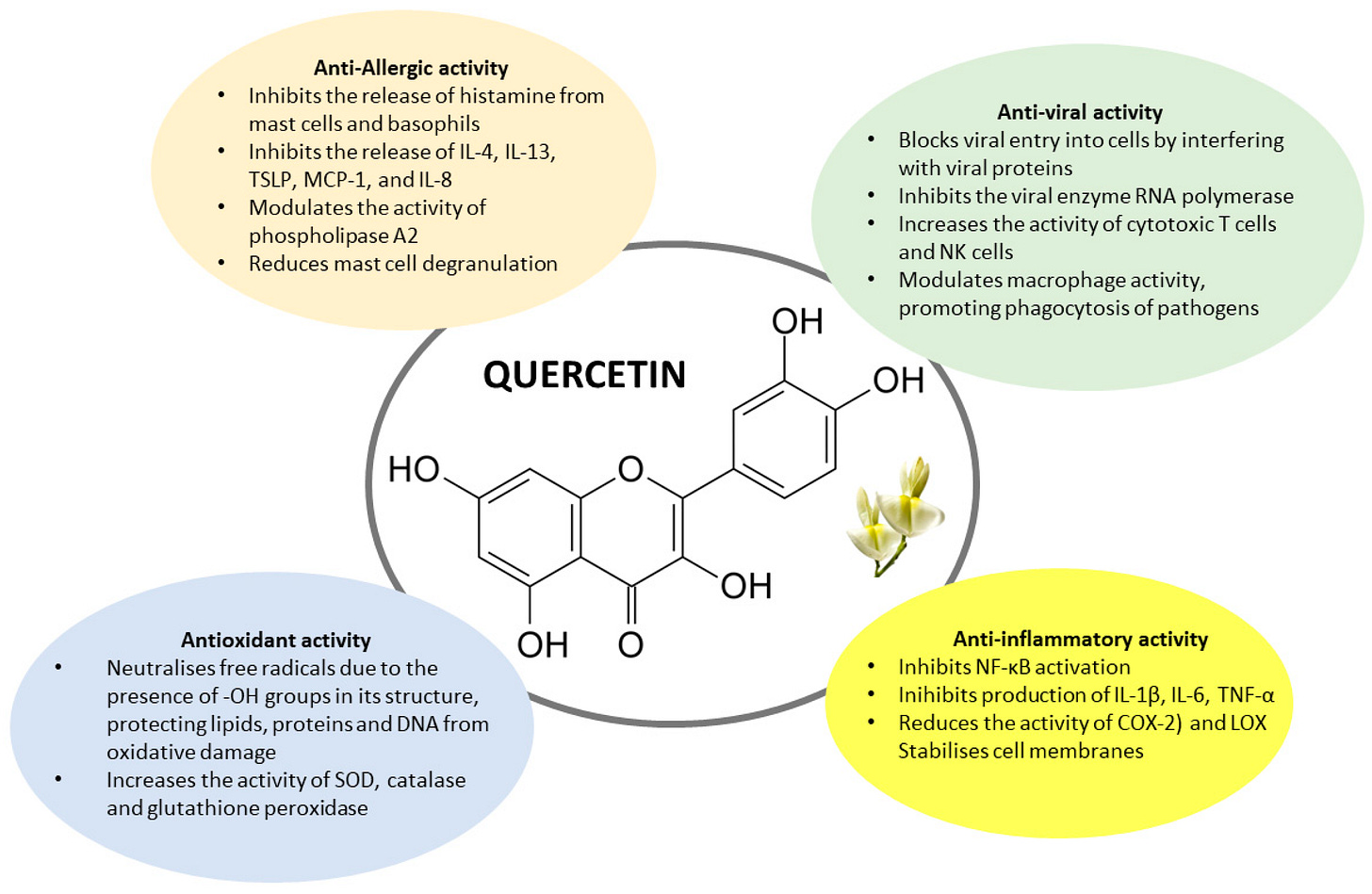
6. Quercetin
Quercetin is a flavonoid with mast cell stabilizing properties in laboratory studies, meaning it may reduce the upstream release of histamine rather than blocking it after the fact.
One 2022 double-blind RCT (66 adults, 4 weeks) found that 200 mg of quercetin phytosome daily significantly improved sneezing, nasal discharge, eye itching, and sleep quality compared to placebo (Yamada et al., 2022). This is a single small study using a specific formulation. Larger trials are needed.
The Protocol:
200 mg quercetin daily (the dose used in this RCT)
Can interact with some medications; check with your pharmacist or doctor before starting
7. Immunotherapy
Immunotherapy gradually exposes the immune system to increasing doses of a specific allergen, retraining it to tolerate pollen rather than overreact to it. It is the only currently available treatment that can modify the underlying disease.
The 2017 EAACI guideline recommended both sublingual (SLIT) and subcutaneous (SCIT) immunotherapy, with a minimum of 3 years for disease-modifying effects. The strongest long-term evidence is for grass pollen tablets (Roberts et al., 2017).
The Protocol:
If standard first-line therapy is not enough, ask for a referral to an allergist and allergy testing to identify your triggers.
They may consider you a candidate for other therapies like immunotherapy.
This is a long-term investment, not a quick fix
Final Thoughts
I started implementing the first five protocols every spring, and the difference compared to my medical school days of suffering through dry mouth and dry eyes is night and day. My allergies have not disappeared, but they have gone from “miserable for weeks” to “occasionally annoying for a few days.” That is a trade I will take every time.
What does your allergy season routine look like? Drop a comment and let me know.
Thanks for reading. If you found this helpful, a like or restack means a lot and helps others discover it.
This newsletter is for educational purposes only. It is not personal medical advice. Opinions are my own. Always consult your own health-care provider for medical guidance.







Great breakdown. One thing worth adding on the bedroom side: dust mites are one of the most common indoor allergens, and they're packed into mattresses, pillows, upholstered furniture, and carpets. They need humidity above 50% to survive, so running a dehumidifier or even just using the exhaust fan after showers can slash your overnight allergen load before HEPA even enters the picture.
The anticholinergic side effects are real, man. I switched to keto a few years ago and noticed my seasonal allergies basically disappeared that first spring - I think the reduced inflammatory response just helped overall. Might be worth mentioning that diet can play a role here since you're already looking at evidence-based approaches.